

The phone call comes at 2 a.m. Your mother has fallen. Suddenly, you're facing a reality you never prepared for: bringing home a parent who can no longer move without help. The hospital hands you a stack of pamphlets, and you realise with a sinking feeling that you're about to become a caretaker for elderly parents, navigating a world of medical equipment and daily care routines.
This guide exists because you shouldn't have to figure this out alone. Whether your loved one is recovering from surgery, managing a chronic illness, or facing the realities of advanced age, the transition to home care is both personal and practical. In this guide, we'll walk through what you need to know, from preventing bedsores to preserving dignity and knowing when professional help is essential. At Heka Health, we believe care should feel like family, and we're here to support yours.
Understanding the unique needs of bedridden elderly care
Caring for a bedridden person means providing constant support for all their daily needs while actively preventing serious medical complications. This state of immobility creates unique risks like pressure ulcers, muscle atrophy, and infections, requiring specialized geriatric care at home that addresses both the physical and emotional challenges for everyone involved.
What does "bedridden" truly mean for daily life?
Beyond the clinical definition, being bedridden reshapes every aspect of existence. Your loved one loses independence in the most basic human functions: bathing, eating, using the toilet, and even shifting position to relieve discomfort. They become dependent on others for tasks they've performed privately for decades.
The psychological toll runs deep. Isolation sets in quickly when someone can't leave their room. Many bedridden patients experience depression, anxiety, and a profound sense of lost identity. The person who once cooked family meals or worked a full career now relies on others for a sip of water.
Common causes include stroke, advanced dementia, severe arthritis, hip fractures, Parkinson's disease, and recovery from major surgery. Understanding the cause helps you anticipate needs and plan appropriate eldercare strategies.
Why specialised care is crucial for preventing complications
Without proper, proactive care, a bedridden person faces serious and preventable medical risks. These complications can develop quickly and significantly impact their quality of life. Informed, consistent care is the best defence against them. That's why knowing the 7 signs your elderly parent needs a professional home caregiver can be a crucial first step.
Complication | Description | Prevention Strategy |
|---|---|---|
Pressure Ulcers (Bedsores) | Painful skin and tissue wounds caused by prolonged pressure on bony areas like the tailbone, heels, and hips. | Repositioning every 2 hours, daily skin checks, using pressure-relieving mattresses. |
Muscle Atrophy & Contractures | Rapid loss of muscle mass and strength. Joints can stiffen into permanently bent positions (contractures). | Daily passive range-of-motion exercises, encouraging small movements. |
Respiratory Infections | Lying flat makes it hard to clear lung secretions, increasing the risk of pneumonia. | Elevating the head of the bed, encouraging deep breaths, ensuring good oral hygiene. |
Blood Clots (DVT) | Deep Vein Thrombosis can form in immobile legs and travel to the lungs, which can be fatal. | Leg exercises, compression stockings, and prescribed medication if needed. |
Urinary Tract Infections (UTIs) | Caused by incomplete bladder emptying, dehydration, or catheter use. | Ensuring proper hydration, timely toileting assistance, and meticulous perineal care. |
Mastering daily routines: hygiene, comfort, and dignity
A structured daily routine is the foundation of quality home care for a bedridden patient. It involves maintaining cleanliness, preventing skin breakdown, and ensuring proper nutrition, all while preserving their sense of dignity. This rhythm of care directly impacts both physical health and emotional well-being.
Gentle bathing and oral care techniques
A bed bath requires preparation and patience. First, gather your supplies: two basins (one for soapy water, one for rinsing), washcloths, towels, mild soap, moisturiser, and clean clothes. Keep the room warm and ensure privacy by only exposing the area you're washing.
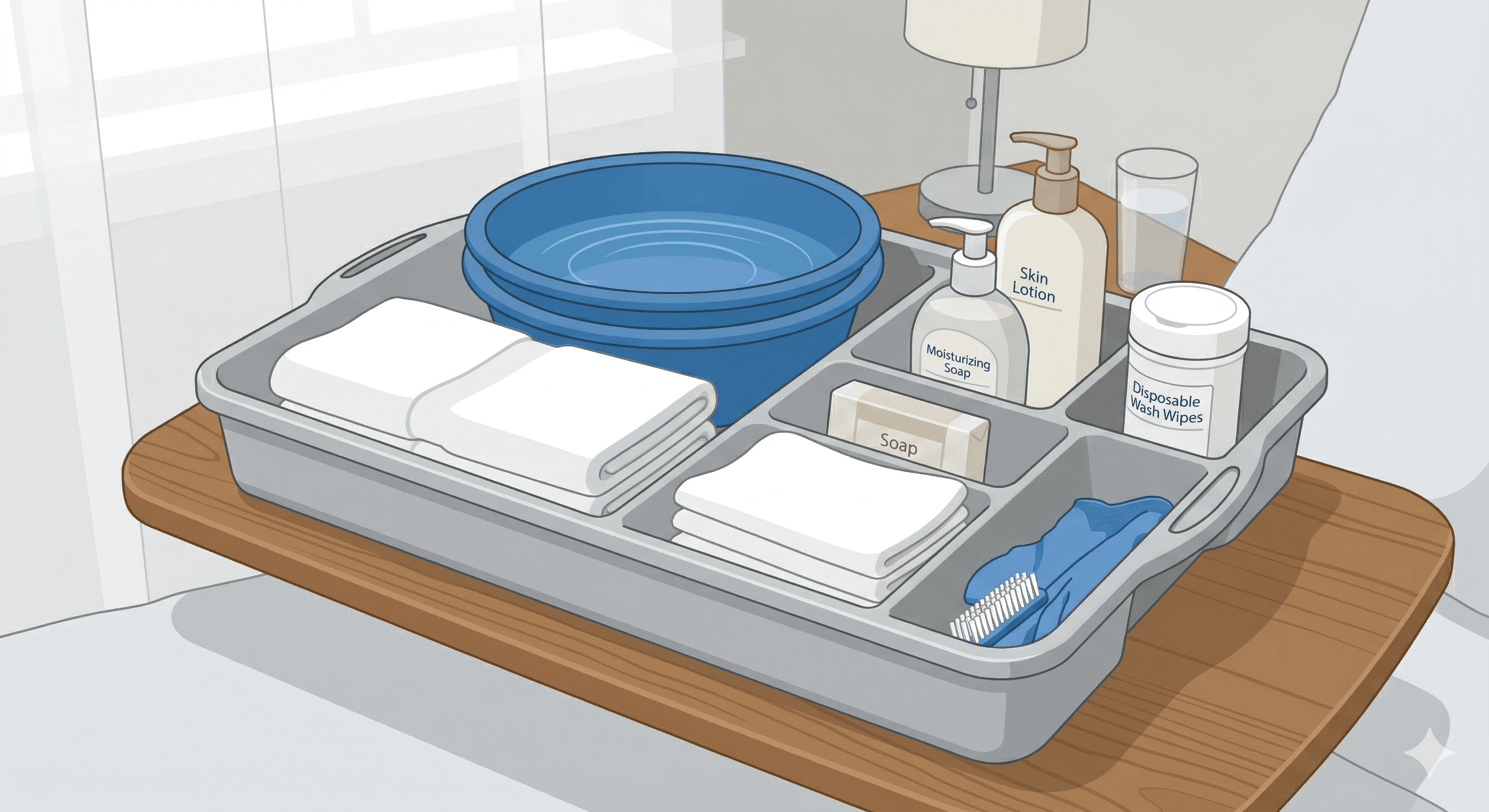
Start with the face using plain water, then work down the body: arms, chest, legs, back, and finally the perineal area. Pat skin dry gently to avoid tears. Apply moisturiser to prevent dryness. Perineal care is vital for preventing infections; always use a clean cloth and gentle motions.
Oral care is more than just comfort; poor oral hygiene can lead to pneumonia. Brush teeth twice daily. If brushing isn't possible, use moistened foam swabs to clean the mouth, tongue, and gums.
Preventing pressure ulcers: positioning and skin care
Pressure ulcers, or bedsores, are a primary risk for bedridden patients. Prevention is centred on a strict turning schedule and diligent skin care. This is a non-negotiable part of daily care that protects your loved one from painful, hard-to-heal wounds.
The two-hour rule is your most important tool: reposition your loved one at least every two hours, around the clock. This means setting alarms at night. Alternate between lying on their back, right side, and left side. Use pillows to support the new position and prevent pressure on bony areas like the hips and ankles.
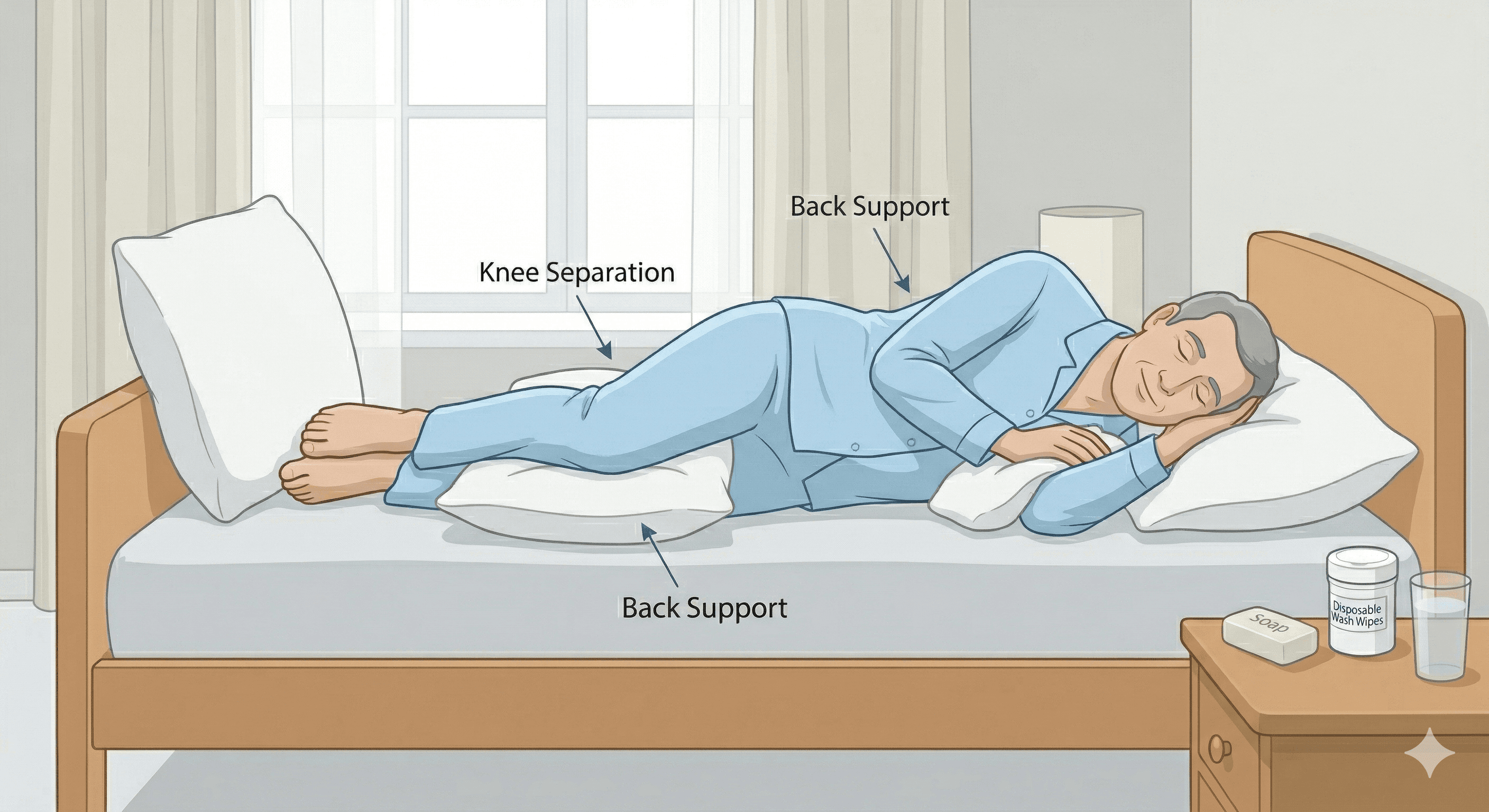
Inspect their skin daily, especially over the tailbone, heels, hips, and shoulder blades. Look for red areas that don't turn white when pressed. This is a stage 1 bedsore and a sign to increase turning frequency. Specialised equipment can make a huge difference. You can explore medical equipment rentals to save money on home care, which makes items like a hospital bed on rent or a pressure-relief mattress more accessible.
Nutrition and hydration: ensuring proper intake
Feeding a bedridden person safely requires careful positioning and patience. Always elevate the head of the bed to at least 45 degrees during and for 30 minutes after meals to prevent choking and aspiration (food entering the lungs).
Swallowing difficulties are common. Watch for signs like coughing during meals, a wet-sounding voice, or pocketing food in the cheeks. If you notice these, consult a doctor. You may need to modify food textures to be softer or thicken liquids.
Offer small bites and allow plenty of time to chew and swallow. Never rush meals. Dehydration is also a major risk, as patients may not feel thirsty or be able to ask for a drink. Offer fluids throughout the day and track their intake. Make mealtimes pleasant with conversation or music to support their emotional well-being.
Supporting mobility and mental well-being from the bedside
Caring for a bedridden patient goes beyond physical tasks. It's just as important to support their mobility where possible and nurture their mental and emotional health. Gentle exercises prevent physical decline, while communication and engagement combat the profound loneliness that can accompany immobility.
Gentle exercises and safe repositioning
Passive range-of-motion exercises are crucial for preventing stiff joints and contractures. This involves you gently moving your loved one's joints through their full range of movement. Perform these exercises daily, moving each joint (shoulders, elbows, hips, knees, etc.) slowly and smoothly 5-10 times. Stop if they feel pain.
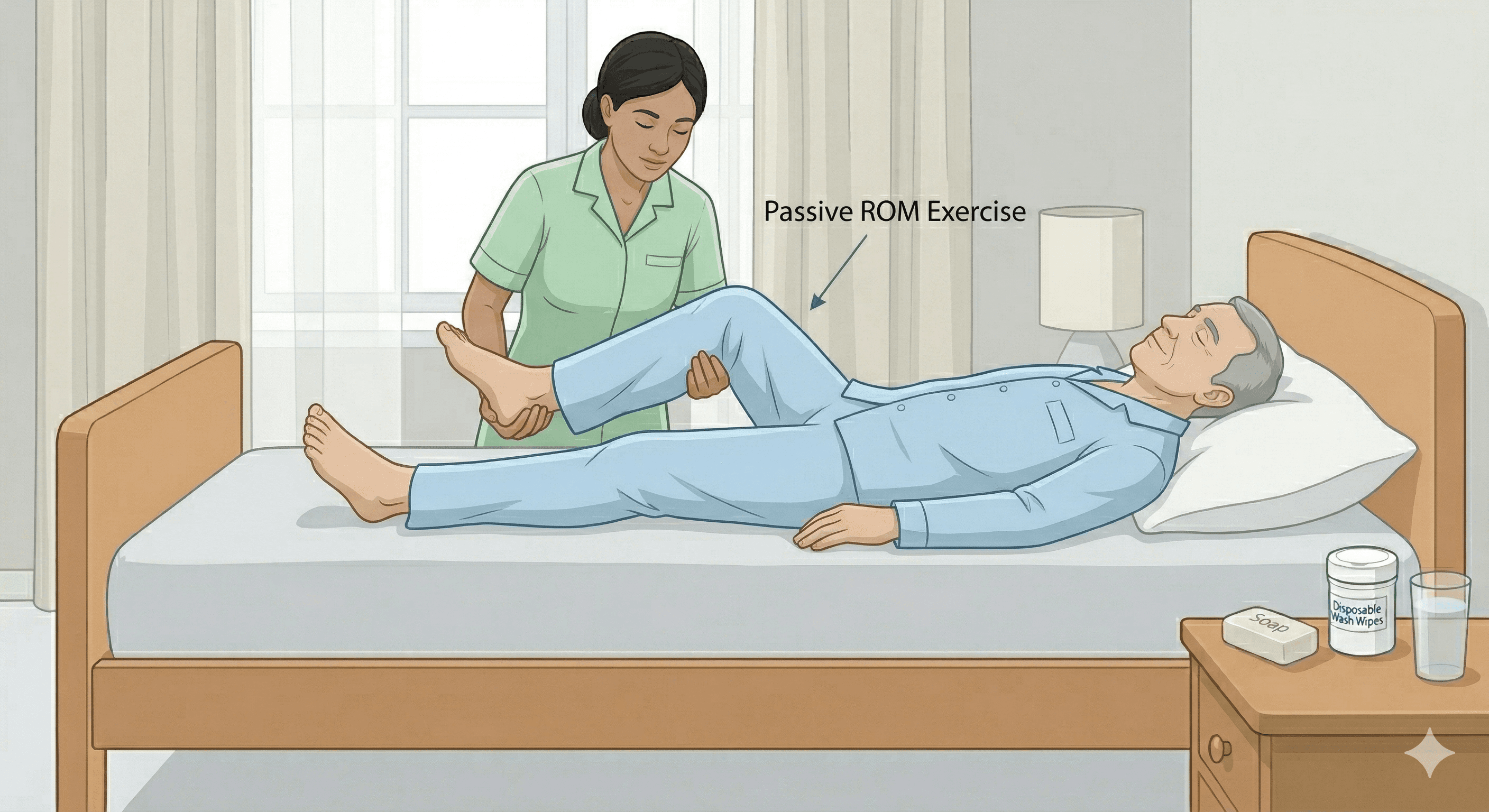
Safe repositioning protects your back. Always bend at your knees, not your waist, and use a draw sheet (a folded sheet under the patient) to slide them instead of lifting. If your loved one needs specialised therapy, professional guidance can be invaluable. For example, home physiotherapy for stroke recovery can provide a tailored exercise plan to maximise function.
Nurturing the mind: communication and engagement
Loneliness is one of the most painful parts of being bedridden. Your loved one's world shrinks to the four walls of their room. You can fight this isolation with intentional connection. Sit at eye level, make eye contact, and ask open-ended questions about their feelings, not just their symptoms.
Engage their mind with activities they can enjoy from bed. Read aloud, play their favorite music, or listen to audiobooks. For patients with cognitive decline, exploring a guide on dementia care at home for 2026 can offer specific communication strategies.
Help them stay connected to the outside world with video calls to family and friends. Position the bed near a window. Most importantly, respect their autonomy by offering choices whenever possible, like what to wear or what to eat. These small decisions restore a sense of control.
When professional help makes all the difference
Recognising when your loved one's needs exceed your family's capacity is a sign of strength, not failure. Professional home care services offer the medical expertise, physical assistance, and emotional respite that family caregivers cannot sustain alone. Knowing the signs of burnout and the benefits of skilled care helps you make the best decision for everyone.
Recognising caregiver burnout and its impact
Caregiver burnout is a state of physical, emotional, and mental exhaustion. It creeps in gradually with symptoms like chronic fatigue, irritability, sleep problems, and feeling constantly overwhelmed. You might find yourself getting sick more often or withdrawing from friends and activities you once enjoyed.
Ignoring burnout doesn't just harm you; it can compromise the quality of care you provide. An exhausted, stressed caregiver is more likely to make mistakes or lose patience. Seeking help is an act of love that protects both you and the person you're caring for. It ensures they continue to receive safe, compassionate support while allowing you to be a daughter, son, or spouse again, not just a caregiver.
The benefits of skilled home care and attendant services
Professional caregivers bring expertise that families can't replicate without training. They know proper transfer techniques, recognize subtle signs of infection, and can manage complex medical tasks like wound care or medication administration. This professional distance can also be a relief for patients, who may feel less embarrassed receiving intimate care from a trained attendant than from their own child.
The respite that professional care provides is essential for sustainability. It allows you to sleep through the night, go to work without constant worry, and tend to your own health. Heka Health addresses the core concerns families face by providing verified caregivers, a fast hiring process, and a replacement guarantee. Whether you need a skilled nurse or a compassionate attendant, our goal is to provide peace of mind. You can learn more with our private nurse for home care hiring checklist or understand the differences in our guide to post-surgery nurses vs. attendants.
Conclusion
Caring for a bedridden loved one at home is a journey of profound love, challenge, and resilience. By focusing on a consistent routine, diligent prevention of complications, and nurturing both body and mind, you can provide compassionate and effective care. Remember to maintain their dignity, offer choices, and celebrate small moments of connection.
Most importantly, remember that you are not alone. Recognising the signs of caregiver burnout and seeking professional help is a crucial part of the process. You don't have to carry this weight by yourself. If you need support, Heka Health is here to provide expert, family-like care, so you can focus on what matters most: being there for your loved one.
Connect with us for support and resources: Facebook, Instagram, YouTube, LinkedIn.
Frequently asked questions (FAQs)
How often should a bedridden person be turned to prevent bedsores?
A bedridden person should be repositioned at least every two hours, day and night. This regular turning relieves pressure on vulnerable, bony areas like the hips, tailbone, and heels, which is the single most effective way to prevent painful pressure ulcers from forming.
What are the early signs of a developing bedsore?
The earliest sign of a bedsore (a stage 1 pressure ulcer) is a patch of skin that looks red or discoloured and does not briefly turn white (blanch) when you press on it. The area may also feel warm, firm, or soft compared to the surrounding skin.
Can a bedridden person still engage in meaningful activities?
Absolutely. Meaningful engagement is vital for mental health. Activities can include listening to favourite music or audiobooks, having conversations with family, looking at photo albums, watching movies, or enjoying a view from a window. Even simple choices, like what to wear, provide a sense of autonomy.
When should I consider professional home care for my bedridden loved one?
Consider professional home care when the medical needs become too complex (e.g., wound care, injections), when you are physically unable to perform tasks like transfers safely, or when you experience signs of caregiver burnout. Seeking help ensures your loved one gets skilled care and you get needed respite.
What medical equipment might be needed for bedridden care at home?
Common equipment includes a hospital bed for easy positioning, a pressure-relief mattress to prevent bedsores, a bedside commode, transfer aids like a draw sheet or slide board, and mobility aids like a wheelchair for any possible transfers. Many families find that exploring medical equipment rentals can save money on home care is a cost-effective solution.
Your well-being
is our priority.
Together, let's navigate every step
with care and compassion.

Your well-being
is our priority.
Together, let's navigate every step
with care and compassion.

Your well-being
is our priority.
Together, let's navigate every step
with care and compassion.
